Is slow, controlled strength training the best form of exercise for people with autoimmune disease? I probably can’t give a truly unbiased opinion on this, as I sell strength training for a living. But I have watched so many clients with autoimmunity benefit from strength training that a deep dive on this subject seems warranted. From Rheumatoid Arthritis to Multiple Sclerosis, proper strength training improves quality of life, pain, function, and body composition. Let’s explore why it’s so effective.
Introduction
Almost everyone benefits from the protection and stability that stronger muscles and bones can give. And people with autoimmune conditions are especially in need of a form of exercise that improves their function without wearing out their joints or leaving them exhausted. This is especially true if the autoimmunity affects joint health directly, as with rheumatoid arthritis. But, beyond the functional improvements, I’m going to propose that proper strength can actually help the body manage the autoimmune condition itself, through the effects exercise in general (and strength training in particular) has on systemic inflammation.
Inflammation and immunity go hand-in-hand.
First, some definitions.
- Inflammation is a state the body creates to promote repair and the removal of pathogens.
- Immunity is the process where special cells identify and destroy potentially dangerous things.
- Autoimmunity is when the immune system treats the body’s own tissues as foreign or dangerous.
During an inflammatory process, a cascade of cellular signals (including chemicals like histamine) makes it easier for white blood cells to get to the pathogen or damaged tissue. Here is an easy way to picture the relationship:

Imagine a waterline ruptures, flooding an intersection. To get it fixed, the city (your body) sets up road cones, caution tape, emergency access lanes, and traffic detour signs (all inflammation) in order to make it easier for the construction and repair crews (immune cells) to access and fix the rupture and removed any damaged piping and concrete.
Needless to say, a problem would develop if inflammation was always “on” and chronic. If road cones and caution tape were everywhere in a city, the repair crews wouldn’t know where to find whatever real problems existed, which would lead to damaged tissues going unrepaired. And, it could also lead to construction crews trying to fix or remove things that didn’t actually need to be fixed (autoimmunity).
Systemic inflammation can lead to autoimmune conditions.
Forgive the simplistic analogy, but the reality is a dizzyingly complex network of signaling molecules. Ultimately what matters is this: systemic inflammation is regarded as a very common pre-cursor of tissue degeneration, immune dysfunction, and autoimmune disease.
“Chronic inflammation is the primary cause of a broad spectrum of diseases, including rheumatoid arthritis (RA), inflammatory bowel disease (IBD; including gastrointestinal conditions such as Crohn’s disease and ulcerative colitis), chronic obstructive pulmonary disease (COPD), asthma, psoriasis and idiopathic pulmonary fibrosis (IPF), among others1.”
Zarin et al, Nature, 2020.
Without going too deep, one way this happens is through the disruption of normal immune cell function. Immune cells function best when they are regularly replaced by new cells, but constant sources of inflammation can prolong the life of existing immune cells like neutrophils. The longer they live, the less well they function, which can lead to them incorrectly identifying our own cells as foreign invaders. Thus, chronic inflammation can trigger auto-immune conditions.
Strength training lowers inflammation directly.
Muscle strengthening exercise lowers inflammation and improves immune function by causing muscles to release special signaling molecules called “myokines.” These myokines exert powerful anti-inflammatory effects. Systemic inflammation is associated with a deficiency of the myokine interleukin-10 (Il-10) which is released by muscle during exercise.
Amazingly, these anti-inflammatory effects can be seen throughout all the organ systems of the body, beyond just the muscles.
- The digestive tract: In one randomized study, endurance and resistance training favorably changed the gut microbiome and inhibited the activation of inflammatory pathways associated with autoimmune diseases.
- The cardiovascular system: Exercise reduces the oxidative stress in the bl and chronic inflammation associated with age.
- The lungs: In COPD patients, Endurance and strength training reduced systemic inflammation and the number of eosinophils, immune cells which become elevated in autoimmune conditions.
- The joints: In patients with RA, regular exercise is associated with lower levels of the inflammatory chemicals TNF-a, CRP, and Il-6.
These are just a few of the hundreds of studies showing that regular exercise in general, and strength training in particular, reduces systemic inflammation. Strength training is a critical step in preventing and mitigating the inflammation which drives autoimmune disease.
Metabolic dysfunction drives systemic inflammation.
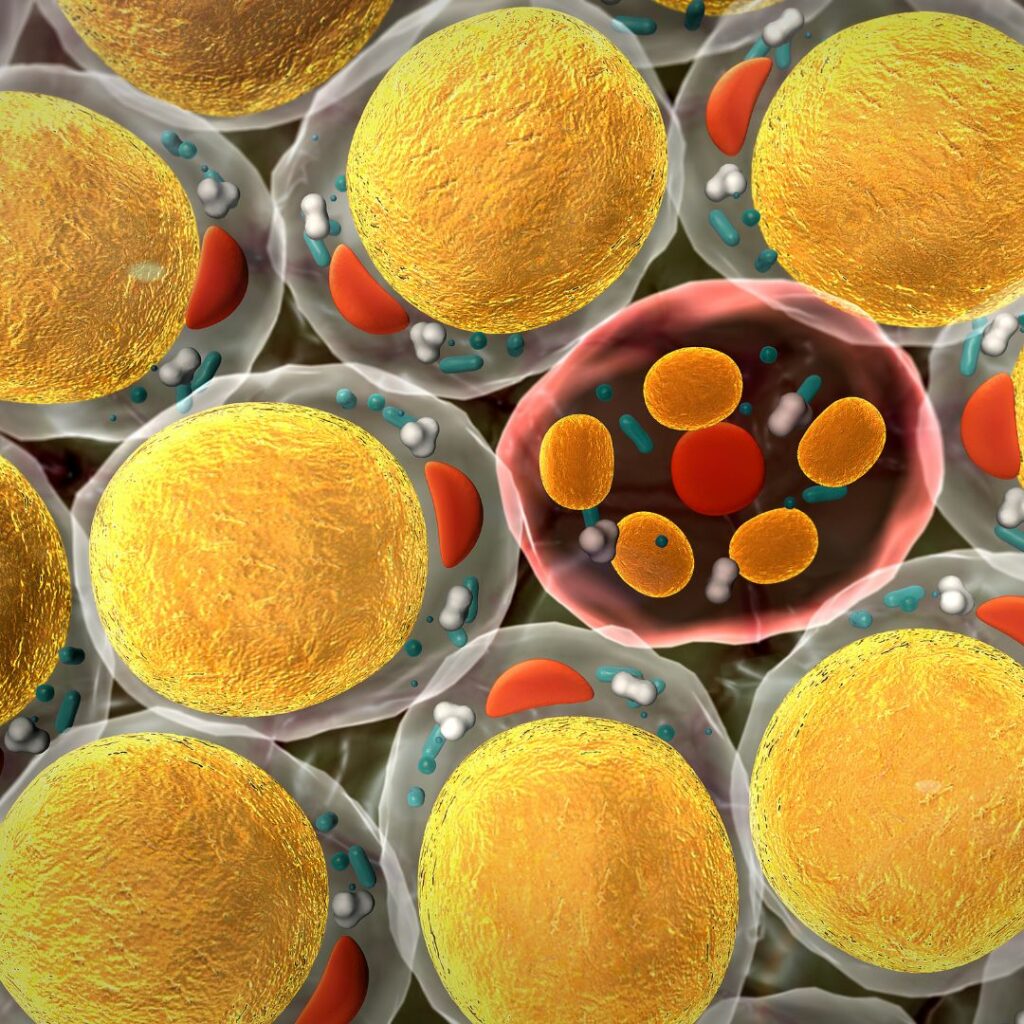
Many people think of their fat cells as these very simple storage containers for extra energy. Far from simple, they are actually quite dynamic, and regulate their stores of energy carefully.
When fat cells reach their capacity and can’t store any more fat, they can enter a cellular state known as “senescence.” They no longer carry on normal processes of gene expression (to avoid becoming cancerous), and begin releasing inflammatory compounds, to include Interleukin-6, designed to get the immune system to come and destroy them. And with pbesity, a perfect storm of systemic inflammation develops which can predispose us to metabolic dysfunction, autoimmune disease, and many cancers.
Strength Training helps prevent and resolve metabolic dysfunction.

Beyond the immediate anti-inflammatory benefits of exercise, regular strength training improves our metabolic health and combats obesity by keeping our metabolic rates high. Muscle is expensive, and by preserving it, we keep the furnace burning and prevent our bodies from suffering the ill-effects of having too much extra energy circulating in the blood.
No amount of exercise can cancel out the effects of overconsuming hyper-processed food. But by regularly engaging in strength training to keep our muscles robust, we can mitigate the damage associated with obesity. Also, high-effort strength training helps regulate hunger signals, and avoids the trap of an out-of-control appetite that other forms of exercise can cause.
Incorporate strength training to both prevent and manage autoimmune disease
Autoimmune diseases are extremely complex problems, and nothing can take the place of a qualified medical care team in their management. But low-force, controlled, safe strength training can play an important role in keeping the body strong, preventing metabolic dysfunction, reducing body fat, and lowering systemic inflammation. All three of these benefits make strength training a crucial part of any effort to reduce our risk of autoimmune disease, or to help optimize our health if we are already trying to manage such a disease.

